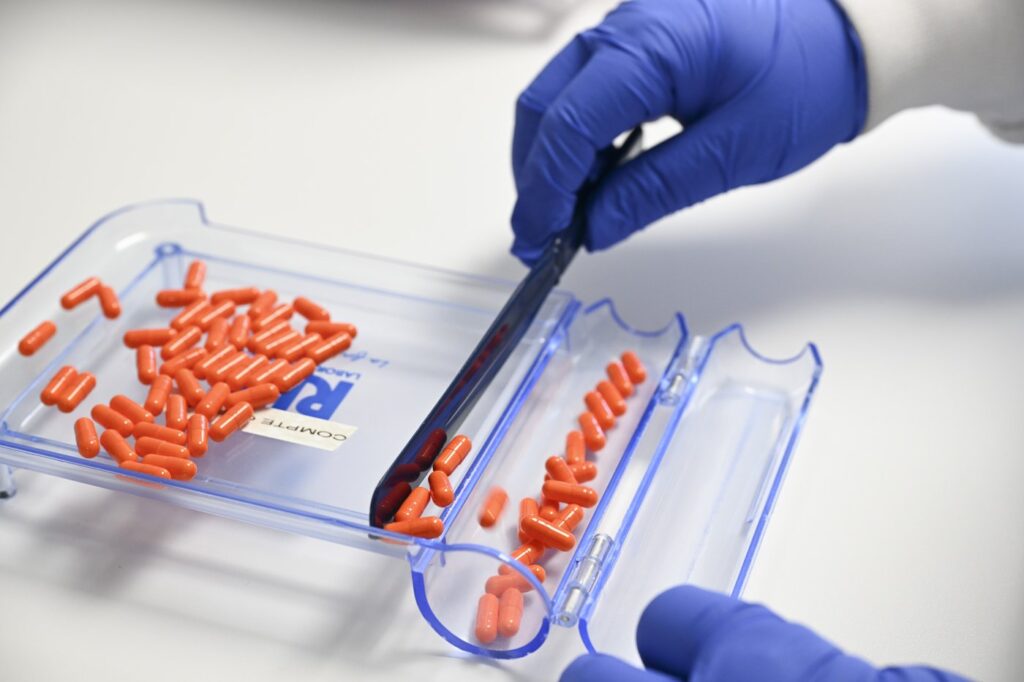
TORONTO — A recent study reveals that the financial burden of medication significantly affects Black Canadians' ability to fill prescriptions compared to their white counterparts. The research, published in the Canadian Medical Association Journal, highlights that Black individuals are less likely to have drug plans that offset medication costs, thereby leading to disparities in healthcare access.
Senior author Bukola Salami states that the findings underscore the impact of socioeconomic inequalities on the health of Black Canadians. The researchers examined data from five years of the Canadian Community Health Survey, finding that approximately 10 to 15 percent of Black adults reported not filling their prescriptions or skipping doses of their prescribed medications. In contrast, only about six percent of white adults reported similar experiences.
Despite controlling for variables such as income and insurance coverage, the disparities persisted, indicating that there are underlying factors affecting Black individuals' healthcare access. Salami speculated that distrust in the healthcare system, potentially stemming from personal or systemic racism, might play a significant role in these findings. She emphasized that while Canada boasts a universal healthcare system, it fails to encompass prescription drug coverage adequately.
The data analyzed was collected prior to the passage of the national Pharmacare Act in 2024. Currently, the federal government has reached agreements to cover diabetes medications and birth control in provinces like British Columbia, Manitoba, Prince Edward Island, and Yukon; however, most provinces and territories have yet to establish pharmacare agreements. Salami expressed the need for additional research to determine whether the introduction of pharmacare will enhance access to prescribed medications for Black Canadians.
According to the study, around 72 percent of Black adults had drug insurance coverage, whereas approximately 80 percent of white adults did. The research utilized data from the Canadian Community Health Survey collected in 2015, 2016, 2018, 2019, and 2022, deliberately excluding the years 2017, 2020, and 2021 due to incomplete data for that period.
Dr. Mojola Omole, president of the Black Physicians Association of Ontario, emphasized the critical nature of these findings. As a breast surgical oncologist who frequently sees Black and racialized patients at Scarborough Health Network, she noted that issues surrounding medication affordability arise "all the time." Omole articulated the harsh reality faced by many individuals, particularly those from a working-class background or who are new immigrants, stating, “If people have to pick between their medication and feeding their families, they’re going to pick feeding their families.”
The study also found that Black patients with insurance were still less likely than white patients to acquire their medications, which could be attributed to a pervasive distrust in the medical system. Omole mentioned, “We have had such long periods where Black communities have not received great care, and even to this day, many have horrific stories of what’s happened to them in terms of the pervasiveness of anti-Black racism.”
The existing primary care shortage exacerbates these issues, as Omole pointed out. The lack of continuity in relationships with healthcare providers, due to absence of family physicians, forces patients to rely on episodic care. This situation complicates their ability to develop trust in healthcare professionals, further impacting their willingness to adhere to prescribed medication regimens.
This study draws critical attention to the intersection of race, socioeconomic status, and healthcare access in Canada. Through highlighting these disparities, the findings reinforce the need for comprehensive strategies to improve medication access and healthcare equity for Black Canadians and other racialized populations.